A research team at Dartmouth’s Norris Cotton Cancer Center has previously shown that fatty particles from the bloodstream may boost the growth of breast cancer cells. They now show that through an unexpected mechanism not previously described in cancer cells, the fat particles bind to the breast cancer cell surface and are then taken into the cell, providing a large supply of fuel that drives proliferation of the cancer cells.
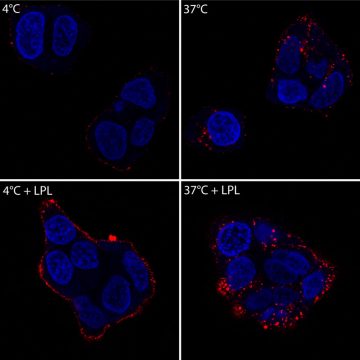
High-fat diets and obesity have been shown to increase the risk of breast cancer and worsen outcomes and prognosis of breast cancer patients. A team of researchers from Dartmouth and Dartmouth-Hitchcock Norris Cotton Cancer Center led by William Kinlaw III, MD, sought to understand how fat from the diet might influence breast cancer cells. In their new study, they found that in addition to making new fat to fuel proliferation, breast cancer cells can take up large quantities of fat derived from the lipid-rich particles that circulate in the bloodstream. The particles bind to the breast cancer cell surface and are then taken into the cell by a novel mechanism not previously described in cancer cells. This uptake provides a large supply of fat that drives proliferation of the cancer cells. Their findings, “Endocytosis of very low-density lipoproteins: an unexpected mechanism for lipid acquisition by breast cancer cells” is newly in press at the Journal of Lipid Research.
“We previously showed that fatty particles in the bloodstream may augment the growth of breast cancer cells,” says Kinlaw. “Our new work demonstrates that breast cancer cells can engulf large amounts of preformed fat from the blood using an unexpected mechanism of fat particle uptake called ‘endocytosis of lipoproteins’.” The uptake results in metabolic reprogramming of the cells to take advantage of this “free lunch” and reveals a direct connection between dietary fat and cancer cell biology.
The literature has also largely focused on manufacture of new fat by cancer cells as a therapeutic target. Many academic- and pharma-based efforts are underway to target the synthesis of new fat by cancer cells. Kinlaw’s work shows that “breast cancer cells can evade being killed by drugs that inhibit fat synthesis by simply taking up more exogenous fat particles,” he explains. The team’s next publication will detail the impact of high fat diets on breast cancer biology in vivo, using mouse models.
William Kinlaw, III, MD, is Active Emeritus Professor of Medicine at Dartmouth’s Geisel School of Medicine, and member of the Cancer Biology and Therapeutics Research Program at Dartmouth’s Norris Cotton Cancer Center. His research focuses on understanding the peculiar metabolic needs of tumors, and how they adjust to them, with an eye toward exploiting tumor metabolism in the clinic. Recent insights relate to the regulation of lipid synthesis in tumors and the ability to target it in preclinical systems and clinical trials.
About Norris Cotton Cancer Center at Dartmouth-Hitchcock
Norris Cotton Cancer Center combines advanced cancer research at Dartmouth’s Geisel School of Medicine with patient-centered cancer care provided at Dartmouth-Hitchcock Medical Center in Lebanon, NH, at Dartmouth-Hitchcock regional locations in Manchester, Nashua and Keene, NH, and Bennington and St. Johnsbury, VT, and at partner hospitals throughout New Hampshire and Vermont. It is one of 51 centers nationwide to earn the National Cancer Institute’s “Comprehensive Cancer Center” designation. Learn more about Norris Cotton Cancer Center research, programs, and clinical trials online at cancer.dartmouth.edu.