Typically, the respiratory immune system clears hundreds of Aspergillus conidia daily, but in immunocompromised individuals Aspergillus conidia can germinate in the lungs leading to the development of invasive aspergillosis. Currently, our knowledge of how Aspergillus fumigatus germination and growth is controlled in the respiratory tract is limited. Phagocytic alveolar macrophages and airway epithelial cells constitute the first lines of defense against inhaled A. fumigatus conidia; subsequently, neutrophils and macrophages are sequentially recruited to the respiratory tract to control fungal growth and germination. But how the antifungal immune response is orchestrated in the respiratory tract after inhalation of A. fumigatus conidia remains ill defined. Our work has highlighted critical roles for leukotrienes, IL-1 cytokine family members, and type I/III interferons is the recruitment and activation of neutrophils and macrophages in the lungs after A. fumigatus challenge. Moreover, we are interested in the cellular and molecular pathway utilized to detect A. fumigatus conidium. Through this work we have identified novel roles for alveolar macrophage sensing of A. fumigatus through the cytosolic receptor, MDA5.
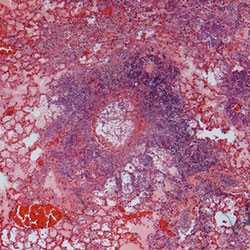
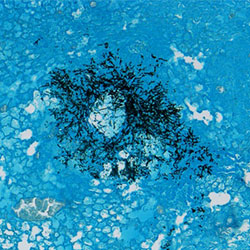
Lung histology stained with H&E (left) and GMS (right) from Kenalog immunosuppressed mice,
which were subsequently challenged with Aspergillus fumigatus (CEA10)
To conduct these studies, our laboratory currently uses gene knockout mice, adoptive cell transfer, bone marrow chimeras, molecular antibody blockade, therapeutic administration of cytokines and chemokines, and immunofluorescent microscopy and flow cytometry to explore the role of these inflammatory mediators in regulating immunity to A. fumigatus. Through these studies, we hope to expand our understanding of how A. fumigatus conidia are typically controlled in immunocompetent mammals with the ultimate goal of developing adjunctive therapies to better treat A. fumigatus infections.