by Mengyi (Zed) Zha
I chose to go to Muhimbili National Hospital for an elective after Match Day and before graduation. I figured this would be a good time to travel as I would have the energy to immerse myself in a new culture. Having grown up and gone through part of my medical training in a resource constrained country, the living condition and lack of resources in the public hospital did not come as a complete shock to me. But how much the patients endure and the challenges to patient advocacy really surprised me.
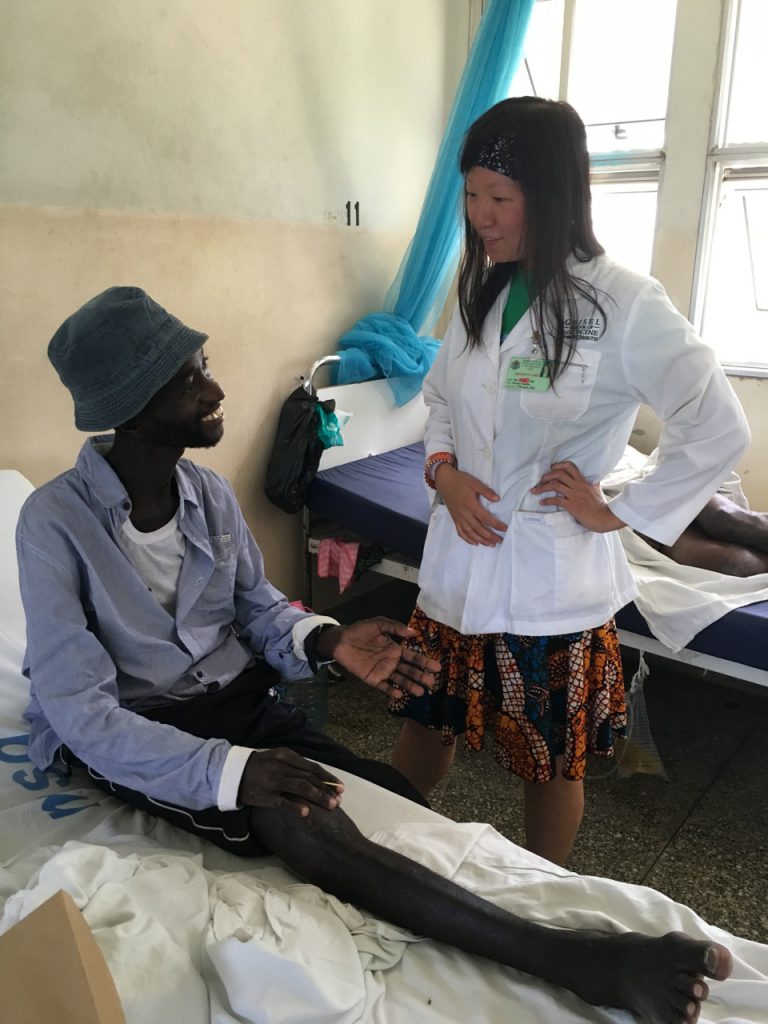
The teaching at Muhimbili National Hospital is great. I felt warmly welcomed by both the faculty and students. The 5th year students took me in as a member of their group right away and we became really good friends. (They even gave me Swahili lessons in exchange of me teaching them Chinese.) I saw so many diseases that I would never have the chance to see in the US. I learned to care for end stage HIV patients, complicated TB and malaria patients in a resource constrained environment. I also spent two weeks in Dermatology, during which I saw many skin manifestations of infectious diseases such as HIV and TB. As part of my career I hope to take care of HIV and TB patients, and this experience has given me a glimpse of what that might look like. I would encourage anyone who is interested in practicing in a low-income setting to take part in this elective. At the same time, Dar es Salaam is a very livable city (despite the intense heat and humidity from being near the equator), and Tanzania is just a beautiful country. I hope I can come back after learning more Swahili.
There was an occasion, however, when my intern and I felt alone and helpless in the fight for the wellbeing of a patient: On a particular national holiday, my intern and I were the only ones from the medical team on the infectious disease ward taking care of over 15 patients, a few of whom were critically ill. This included a patient with stage IV AIDS and PCP lung infection, for whom I had been pushing to transfer to the ICU for days. I put the patient on 15L of O2 the previous day so that his oxygen saturation was over 90 percent. On this day when I showed up in the morning, the patient’s oxygen tank was empty because it had run out overnight and there was nobody to change it, leaving his oxygen saturation very low. After transferring and changing the tank myself, the patient was still only saturating in the low 80s. My efforts to transfer the patient to the ICU continued to fail due to his terminal status. The patient deteriorated throughout the morning and arrested during the lunch hour (a busy time when family typically visits). Our resuscitation efforts were challenging due to lack of nursing staff; several times I had to stop chest compression to search for medications and proper devices. The patient passed away. The family broke down crying, and so did I. It was through such emotional turmoil that I have developed a heart for the patients and their families.
This elective is generously supported by a grant from the Hanover Rotary Club.
