This never happens. Pediatric patients don't get airlifted anywhere in Rwanda, but nevertheless: there's the Air Force helicopter, idling behind King Faisal Hospital in the heart of Kigali after its trip from Butare Hospital, about 75 miles south of the capital.
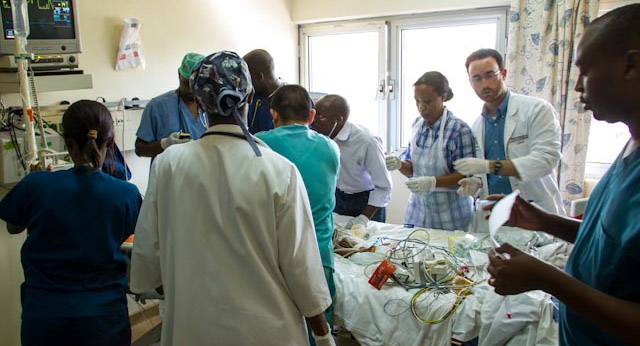
Dorey Glenn, MD, Geisel School of Medicine Pediatrics Instructor and DHMC residency graduate, is trying to find the patient. When at last he tracks her down, the three-year-old girl is coding in the emergency room. The room is clean, tidy, and fairly well equipped, and the girl's bed is surrounded by an assortment of medical personnel. One of them is Dr. Elie Niyibizi, Dr. Glenn's “twin” (Rwandan counterpart) in the Human Resources for Health program that started this summer and which includes a handful of Dartmouth faculty.
Dr. Elie graduated residency last year, and while there is a lot of variation in the quality of medical professionals in Rwanda, Dr. Glenn explains that Dr. Elie has developed himself into a fantastic physician. Dr. Glenn says he often asks himself how Dr. Elie came out of the same residency program as all the others, but somehow managed to gather the knowledge, the experience, and the excellent clinical decision making skills that he consistently displays. “If it wasn't for him,” says Dr. Glenn, “I think my experience here would be totally different.”
Which goes a long way towards explaining why Dr. Glenn feels no need to get in front of his twin and call the shots. In part, of course, running a code is the job of the ER team, and the HRH faculty are supposed to refrain from stepping in and taking over. Their Rwandan counterparts should take charge, so Dr. Glenn mostly watches as the team of Rwandan physicians try to resuscitate the girl. In vain, as it turns out.
Sadly, that happens a lot, explains Dr. Glenn later. King Faisal's 25-bed pediatric ward sees a couple of deaths per week. Even with the best facilities in the country, if a patient at King Faisal is as far gone as the girl in the ER, they rarely survive. Part of what's so different compared to U.S. medical centers, says Dr. Glenn, is the level of backup – here, there is none. King Faisal Hospital is the referral hospital's referral hospital: if their team and their resources can't cut it, then it's the end of the line.
While a student or resident in a Dartmouth clinical setting would not get to see or experience many actual codes, there would have been plenty of clinical simulations from which to learn from. In Rwanda, Dr. Glenn encourages his colleagues and the pediatric residents and medical students to use situations like the code in the emergency room to learn and practice. A further learning opportunity will present itself with the mortality and morbidity discussion of the code and its outcome that Dr. Glenn will help conduct as part of his work to strengthen the quality of Rwanda's health care system.