Tshibambe Nathanael Tshimbombu MED’24, served as lead, Geisel student author of two manuscripts bolstering health and healthcare in his home country of the Democratic Republic of Congo (DRC), which have been impacted by continuous military conflicts and political instability, as he points out.
Blog
The Center Welcomes its First DarDar Medical Exchange Students From Tanzania Since the Pandemic
The Center for Global Health Equity (CGHE) welcomed its first international exchange students since the 2020 pandemic halted global health programs worldwide. David Muhunzi and Stella Kaihula arrived in Hanover last August as part of the DarDar bilateral exchange program between Muhimbili University of Health and Allied Sciences (MUHAS) in Dar es Salaam, Tanzania, and Dartmouth College.
CGHE Celebrates 10th Anniversary
On Friday, October 27th we celebrated CGHE’s 10th anniversary! Over the past decade, CGHE has made significant strides in promoting global health equity through research, education, and outreach in historically underserved communities.
Dartmouth Medical Student’s Quest for Answers to Big Questions in Global Health
It’s often difficult to understand how a certain experience will shape your future, but for Carly Ratekin MED’25, her work with the Lwala Community Alliance’s maternal and child healthcare program in Kenya felt pivotal from the start.
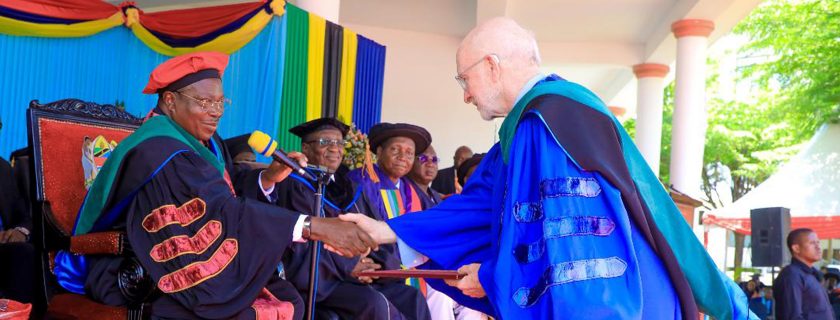
Tanzanian Partner Honors DarDar Director – Dr. Ford von Reyn
DarDar International Programs Director Ford von Reyn receives an honorary degree for his contributions to public health in Tanzania.
DarDar Back in Swing
The DarDar bilateral medical student exchange program between the Geisel School of Medicine and Muhimbili University of Health and Allied Sciences in Dar es Salaam, Tanzania, resumed after a brief pause due to the pandemic. Izhar Mbarani MED ’22, Kate Miller MED ’22, and Sathvik Namburar MED ’22, participants in The James Stickler Clinical Elective in Global Health, and Sara Ratican, MED ’22, The Ford von Reyn Research Elective, traveled to MUHAS in April and spent four weeks immersed in Tanzanian healthcare and culture.
Dartmouth Alumni Inspires Future Doctors and Public Health Professionals
Dr. Maryam Amour, MD, MMed, MPH (’15), Dartmouth Alumni and global health expert, inspires future doctors and public health professionals.
Center for Global Health Equity Awarded Margo Krasnoff Grant for Global Nutrition Scholarships
The Center for Global Health Equity (CGHE) is delighted to announce it is the recipient of a $4800 grant from The Margo Krasnoff Fund for Global Health and Nutrition.
On the Passing of Paul Farmer
On the Passing of Paul Farmer – Lisa V. Adams remembers the global health pioneer’s generosity with his patients, his learners, and his colleagues.
Global Oncology Fellowship Elective Impacts Collaborations in Cancer Care and Knowledge Exchange
For the past two years, fellows from the Dartmouth-Hitchcock Hematology-Oncology Fellowship Program have been engaged in a global oncology fellowship elective in Rwanda.